Analyzing how chronic cortisol elevation suppresses T-cell production and the evidence-based methods to reverse the impact.

Cortisol is often disparaged as the "stress hormone," yet it is a fundamental survival mechanism essential for human life. Produced in the adrenal cortex, cortisol follows a diurnal rhythm, peaking in the morning to provide energy and tapering off at night to allow for restorative sleep. However, when the body perceives a constant threat—whether physical or psychological—this rhythm is disrupted, leading to systemic consequences for the immune system.
In the short term, cortisol is actually an anti-inflammatory agent. During an acute "fight or flight" response, cortisol suppresses non-essential functions to focus energy on immediate survival. One of these suppressed functions is the inflammatory response. This is why synthetic cortisol (prednisone) is used to treat autoimmune flare-ups.
The paradox arises with chronicity. When cortisol levels remain elevated for weeks or months, the immune system’s white blood cells develop a "resistance" to it. This leads to a state of chronic, low-grade inflammation because the cortisol can no longer effectively signal the immune system to "shut off" its inflammatory response once a threat has passed.
The most direct impact of chronic cortisol elevation is on the adaptive immune system, specifically T-lymphocytes. High levels of glucocorticoids inhibit the production of Interleukin-12, a signaling molecule critical for the activation of Th1 cells.
These Th1 cells are the body’s primary defense against viruses and intracellular bacteria. When cortisol disrupts this pathway, the body becomes significantly more susceptible to:
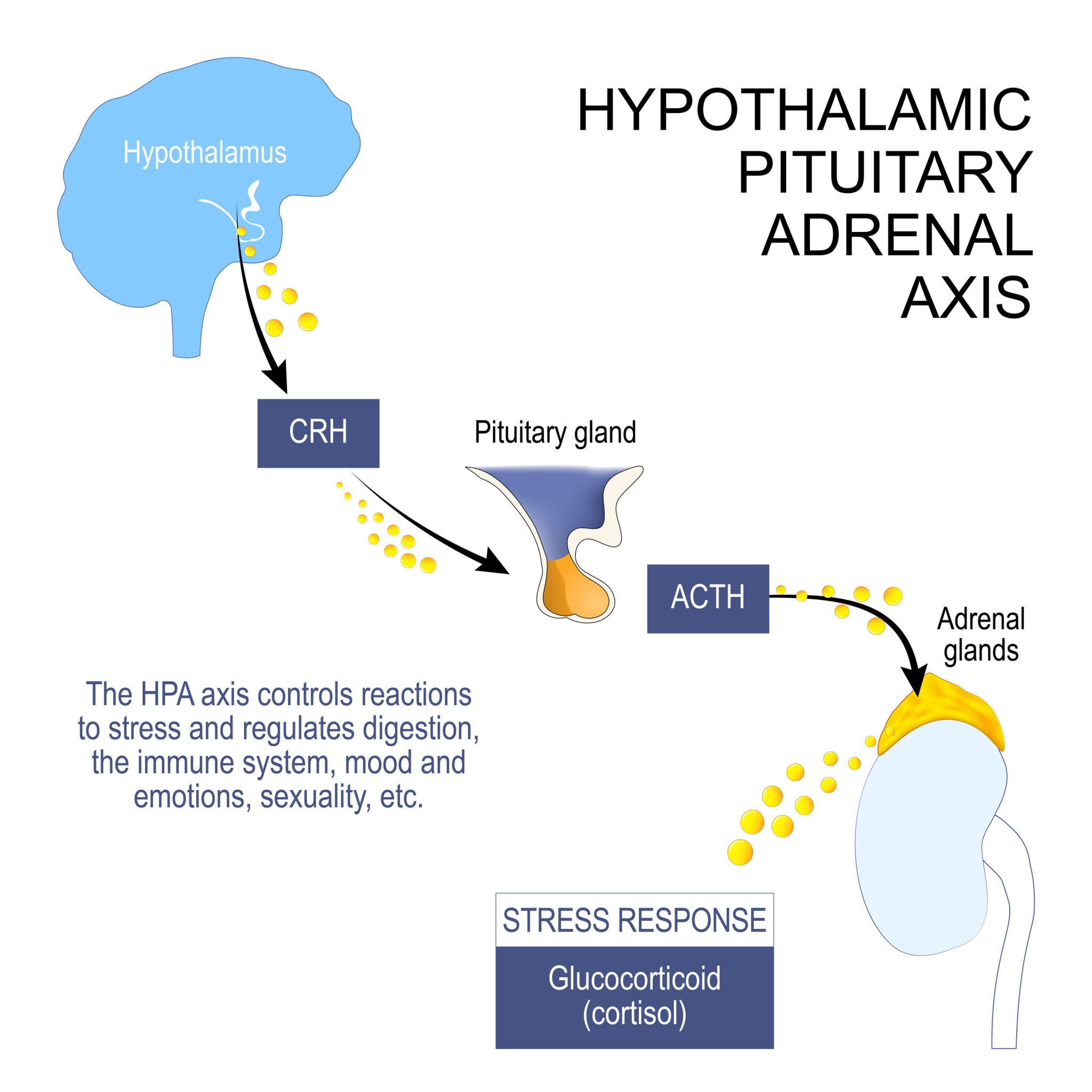
The Hypothalamic-Pituitary-Adrenal (HPA) axis is the control center for the stress response. When the hypothalamus detects stress, it sends a signal to the pituitary gland, which then prompts the adrenal glands to release cortisol.
In a healthy system, a feedback loop exists: high levels of cortisol eventually signal the hypothalamus to stop the stress response. In chronic stress, this feedback loop breaks. The brain loses its sensitivity to cortisol, and the adrenal glands continue to pump out the hormone even when no physical danger is present. This "open loop" state is a primary driver of modern lifestyle-related diseases, including metabolic syndrome and anxiety disorders.
Regulating cortisol is not about eliminating stress—which is impossible—but about restoring the feedback loop of the HPA axis. Scientific literature supports several non-pharmacological interventions that have a measurable impact on serum cortisol levels:
Phytotherapeutic SupportSpecific plants known as "adaptogens" have shown promise in clinical trials. Substances like Ashwagandha (Withania somnifera) have been observed to reduce morning cortisol levels by up to 30% when used consistently over an eight-week period.
Sleep Hygiene and Circadian AlignmentBecause cortisol is tied to the light-dark cycle, maintaining a consistent sleep schedule is the most effective way to reset a dysregulated HPA axis. Exposure to natural sunlight within 30 minutes of waking helps set the "cortisol awakening response," ensuring the hormone peaks and drops at the correct times.
Understanding the science of cortisol shifts the conversation from "avoiding stress" to "managing physiology." By recognizing how this hormone interacts with the immune system at a cellular level, individuals can implement targeted strategies—ranging from nutritional support to circadian timing—to protect their long-term health from the corrosive effects of chronic activation.